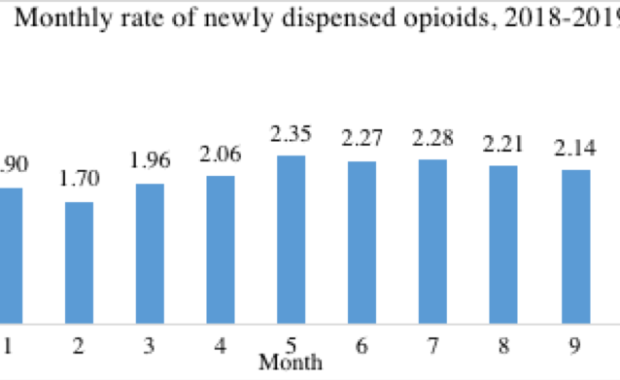
Our new study published in the Canadian Journal of Addiction found plateauing rates of new starts of opioid analgesics in British Columbia in
Improving opioid agonist care continuation, meta-analysis
Improving opioid agonist care continuation remains to be a challenge for many community based addiction treatment organizations. Research into
This changed my practice
Can We Identify Patients at Risk for Opioid Use Disorder when Beginning Opioid Analgesics for Pain from New or Ongoing Non-cancer Causes? There is
Expanding opioid agonist therapy while learning from HIV/AIDS
Accessing opioid agonist therapy (OAT) and maintaining good adherence faces many barriers which can be geographical, financial, regulatory,
Towards a research agenda for addiction education in Europe, u21 poster
u21 health sciences group 2020 virtual meeting: A collaborative approach to healthcare was hosted by University College Dublin from August 25th -
Can prescribers avoid contributing to opioid use disorder?
A 21 y/o has surgery for a condition expected to improve. He fills a discharge prescription for 5 days of an opioid at a standard dose. At 1-week
Hospital based opioid agonist treatment
Researchers recently found that many people with co-occurring mental health and substance use disorders are admitted to inpatient psychiatric units.
Pain Management with Opioids in 2019-2020
This JAMA Insights Clinical Update reviews evidence-based use of opioids to manage noncancer pain, proposing opioid-sparing pain management. Based on
America could relax opioid treatment access policies
Canada and the United States (U.S.) face an opioid use disorder and opioid overdose epidemic. The most effective OUD treatment is opioid agonist