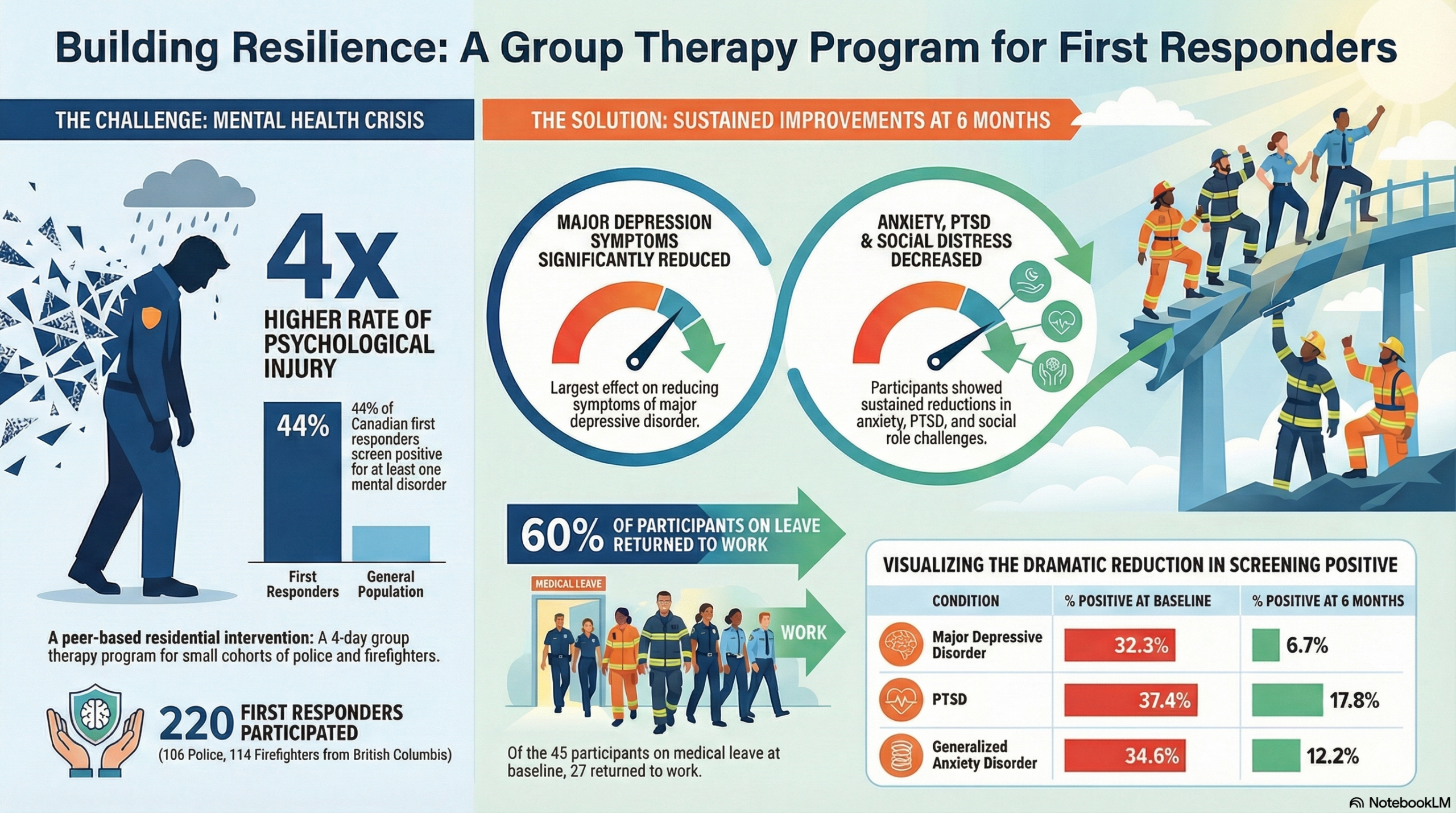
This blog summarizes the results of a recent study published in Comprehensive Psychiatry evaluating the First Responder Resiliency Program (FRRP). 220
Tramadol blasts from the past
The world looks different today than in August 2020. Hunkered down, some of us took the time to look into the evidence on opioid analgesic
Study recommends moving beyond opioid sparing
BC learns lessons from opioid prescribing portraits, new primary care study says. What is the study about? This study was part of a rigorous
20 years qualitative research interviewing
I first interviewed a person with lived experience of substance use twenty years ago. Today, I wanted to pause and reflect on the key points in this
Connecting professionals to promote interdisciplinary trauma-focused therapy
Connecting professionals can promote interdisciplinary trauma-focused therapy and return-to-work support for clients with work-related PTSD. This blog
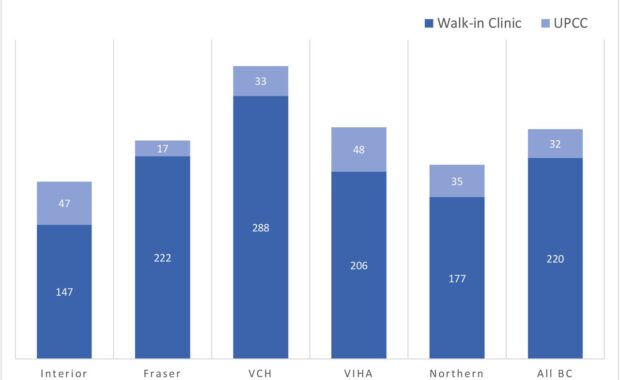
Comparing Walk-in Clinics and Urgent Primary Care Centers
Walk-in clinics are non-hospital based primary care facilities that are designed to operate without appointments and provide increased healthcare
Group therapy alleviates psychological distress in prostate cancer
Emerging evidence that group therapy helps men with prostate cancer.
Dennis McCarty receives prestigious Kentucky award 2022
Dennis McCarty, Ph.D., an Emeritus Professor in the School of Public Health at the Portland State University and Oregon Health & Science
Why inequality hinders effective pain relief for opioid naive people
Equitable access to care is problematic; some people get it, most are left out. The REDONNA study (https://doi.org/10.1016/j.cct.2021.106462) began