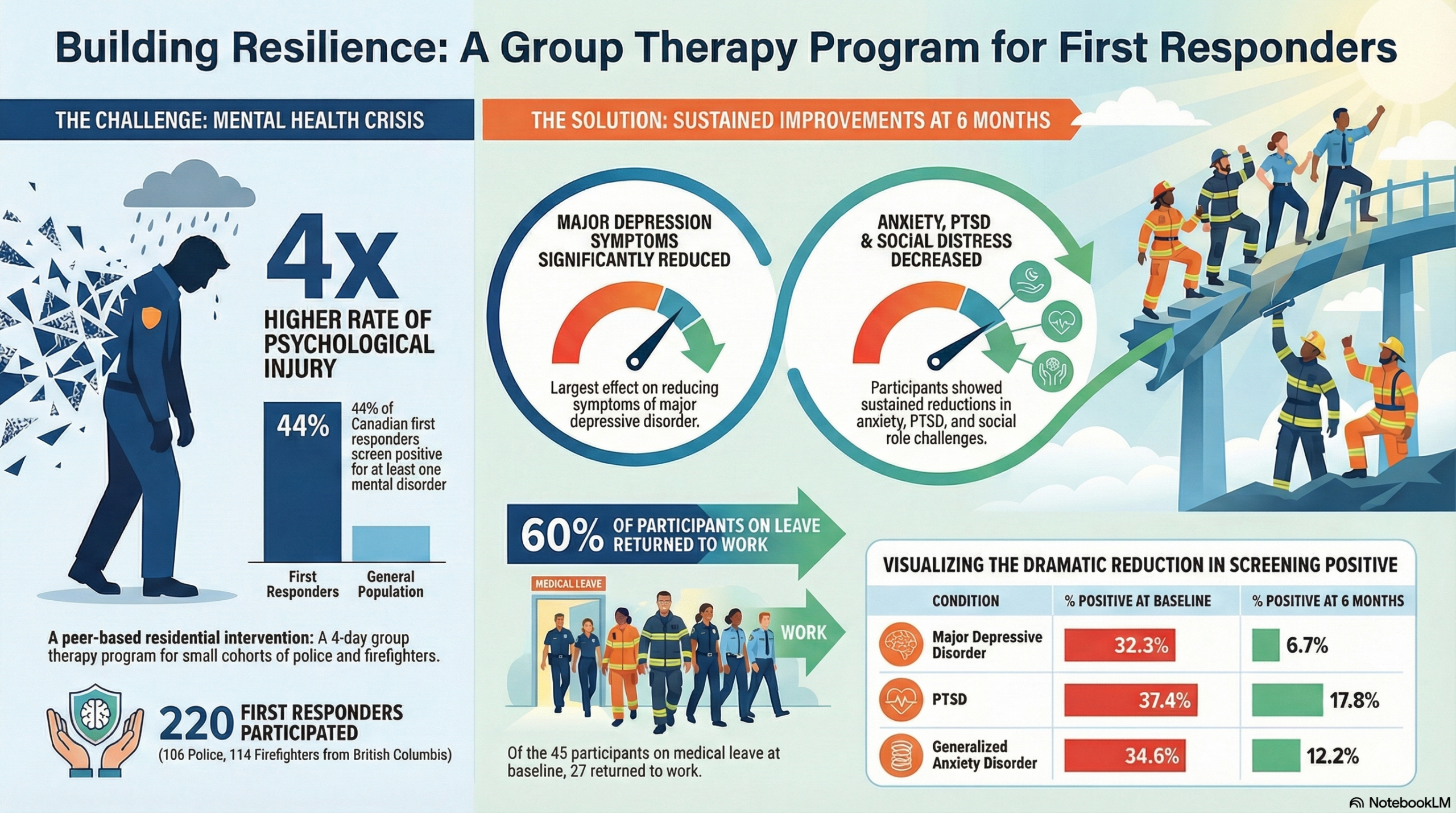
This blog summarizes the results of a recent study published in Comprehensive Psychiatry evaluating the First Responder Resiliency Program (FRRP). 220
Connecting professionals to promote interdisciplinary trauma-focused therapy
Connecting professionals can promote interdisciplinary trauma-focused therapy and return-to-work support for clients with work-related PTSD. This blog
Group therapy alleviates psychological distress in prostate cancer
Emerging evidence that group therapy helps men with prostate cancer.
Dennis McCarty receives prestigious Kentucky award 2022
Dennis McCarty, Ph.D., an Emeritus Professor in the School of Public Health at the Portland State University and Oregon Health & Science
Where science meets meditative solutions
Tired, overwhelmed, or stressed out? Worried about the future and what it may bring? Then join us for the Spring Session of an 8 week meditation
Modernizing withdrawal management services, review
Withdrawal management remains one of the essential skills of addiction medicine specialists. This review describes the recent clinical advances and
Male Pain and Alcohol
Pain is a universal experience across people of all genders. How do we know when something hurts inside? It keeps coming back; first, it disrupts,
Can prescribers avoid contributing to opioid use disorder?
A 21 y/o has surgery for a condition expected to improve. He fills a discharge prescription for 5 days of an opioid at a standard dose. At 1-week
Hospital based opioid agonist treatment
Researchers recently found that many people with co-occurring mental health and substance use disorders are admitted to inpatient psychiatric units.